
Patients are falling behind on medical bills, and collection agencies managing healthcare portfolios are feeling the impact. Medical debt is linked to roughly 66.5% of bankruptcies in the U.S., showing how quickly unpaid balances escalate.
Consumers are often overwhelmed, disengaged, and unsure how to respond, making recovery harder for third-party agencies and increasing compliance risk under frameworks like Regulation F.
This is where omnichannel debt collection for healthcare changes the equation. In this article, we explore how connected communication, automation, and consumer-first engagement can improve recovery rates and reduce friction across the payment process.
A recent study found that within 18 months of a traumatic hospitalization, the share of patients with debt in collections increased by 5.2 percentage points, a 24% relative rise compared to pre-treatment levels. This shows how quickly financial strain compounds when accounts move into third-party collections without clear, timely communication.
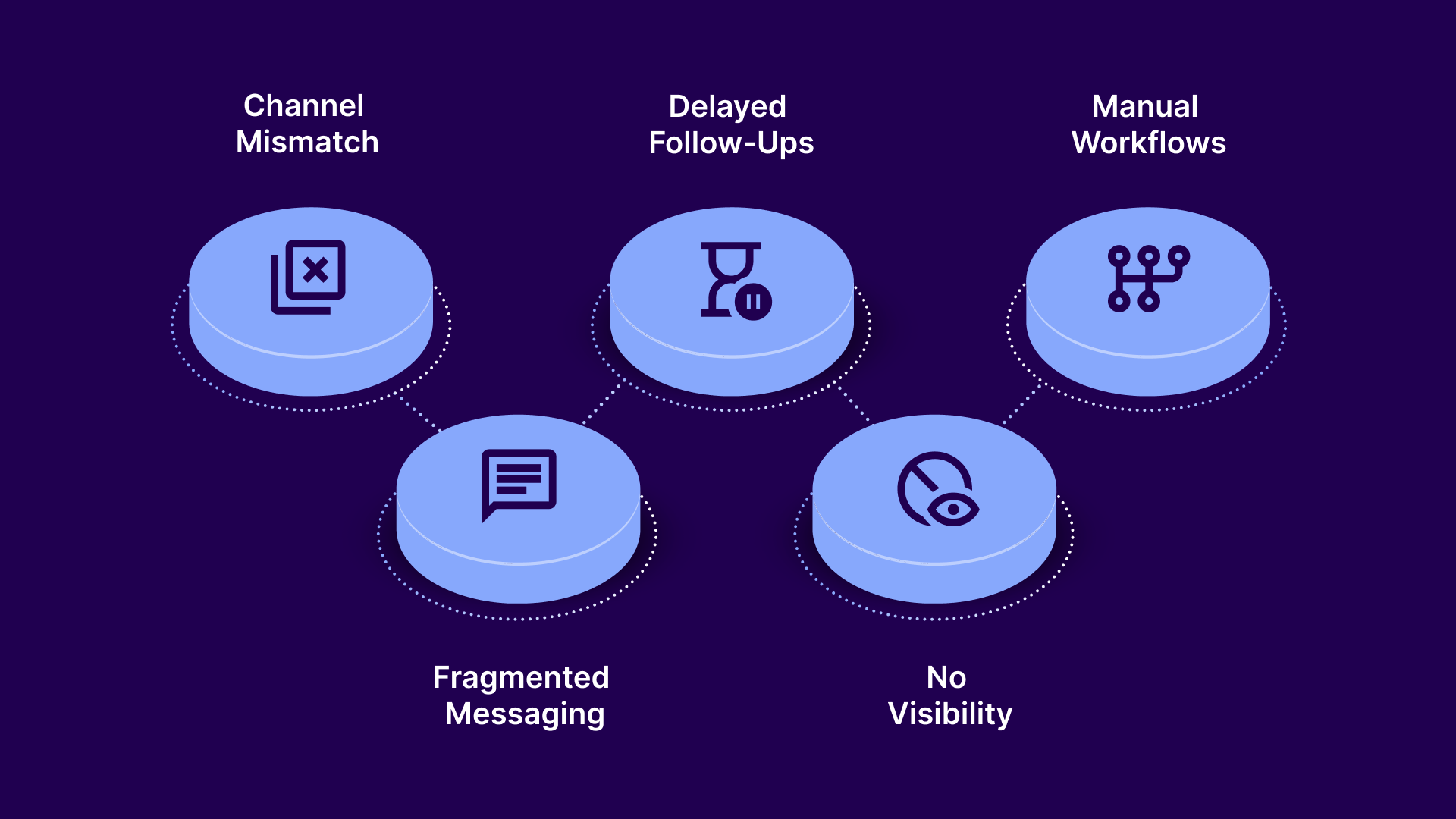
These are the common challenges that reduce consumer payments:
Users do not engage uniformly across channels, yet outreach strategies often remain static. When communication fails to meet account holders where they are most responsive, messages are ignored, and payment opportunities are lost.
Patients receive disconnected messages across calls, emails, and letters with no continuity. This lack of coordination creates confusion and reduces trust in the payment process.
Long gaps between outreach attempts weaken urgency and reduce the likelihood of action. Without timely reminders, consumers are more likely to prioritize other matters or forget outstanding balances.
Teams cannot track a complete history of user interactions across systems. This results in repetitive or conflicting communication that frustrates consumers and delays resolution.
Outreach processes rely heavily on manual effort, limiting scale and consistency. As account volumes grow, teams struggle to maintain timely and effective communication.
Disconnected outreach directly impacts recovery outcomes. In the next section, we break down the approach that brings structure, consistency, and better results to healthcare collections.
Suggested Read: Omnichannel Debt Collection Outreach Automation Guide for Higher Recovery
Omnichannel debt collection connects every patient touchpoint into one coordinated experience. It ensures communication is not just multi-channel, but aligned, timely, and consistent across the entire payment process. The goal is simple. Reach account holders where they respond and make it easy for them to act.
Here is what that looks like in practice:
Tratta operationalizes this approach by combining SMS, email, voice, IVR, and digital touchpoints into a single system. It enables personalized, behavior-driven campaigns, smart channel routing, and real-time tracking to deliver messages when and how account holders are most likely to respond. Schedule a free demo today.
Expectations have shifted, and collection strategies need to keep up. A McKinsey study found that 76% of consumers get frustrated when interactions are not personalized, which directly impacts engagement and payment behavior.
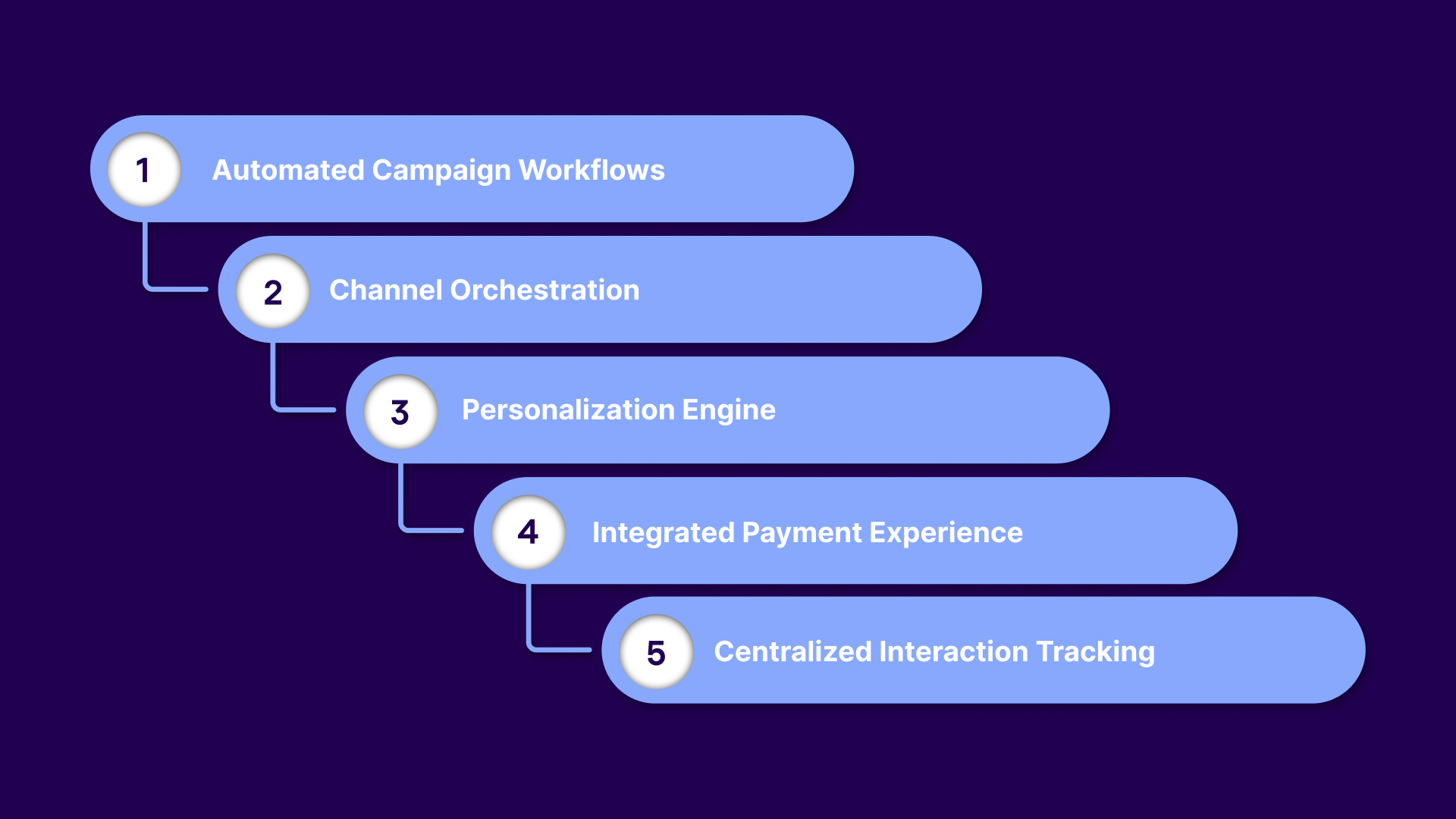
For collection agencies managing healthcare portfolios, omnichannel debt collection improves recovery by combining the right components with the right execution. This is how it works:
Automation ensures outreach happens at the right time without relying on manual effort. It keeps communication consistent across the entire collection lifecycle. This helps agencies maintain momentum and avoid missed opportunities.
Here is how this improves recovery:
Omnichannel systems coordinate how and when each channel is used. This ensures users receive messages in the format they are most likely to respond to. It removes the randomness from outreach strategies.
Here is how this drives better outcomes:
Personalized communication makes outreach more relevant and actionable. It ensures consumers receive messages that reflect their situation and history. This reduces friction and improves engagement.
Here is what this enables:
Omnichannel systems connect communication directly to payment options. This reduces the number of steps patients need to complete a transaction. It shortens the path from intent to action.
Here is how this increases recovery:
A combined view of all user interactions ensures communication remains consistent. It eliminates duplication and confusion across channels. This creates a smoother experience for both patients and teams.
Here is how this helps healthcare portfolios:
These components show that recovery improves when systems are structured rather than fragmented. In the next section, we look at how to design communication flows that guide patients from first contact to final payment.
Suggested Read: How Payment Communication Software Improves Debt Recovery
In healthcare collections, patients move through stages, from awareness to decision to payment. Designing communication flows means aligning each touchpoint to that journey so consumers know what to expect and how to act.
This is how you can use omnichannel communications to design a high-recovery strategy:
This is where users first become aware of their balance. The focus is on clarity and visibility, not urgency. It sets the base for engagement.
Here is what this stage should include:
At this stage, account holders are evaluating their options. They need more context and flexibility to move forward. Communication should reduce uncertainty.
Here is how this stage should work:
This is where intent is highest, and action should be immediate. Communication should remove all friction and make payment simple.
Here is what this stage should enable:
Not all consumers act immediately. Timely reminders help maintain urgency without overwhelming them. This keeps the account active.
Here is how reminders should function:
Once payment is made, communication should shift to confirmation and closure. This improves the overall patient experience. It also reduces unnecessary follow-ups.
Here is what this stage includes:
Tratta enhances omnichannel communication by combining transparent billing, detailed account visibility, and real-time verification across every touchpoint. With flexible payment plans and configurable settlement offers embedded into outreach, patients understand their options clearly and act faster. Call us to learn more.
Implementing omnichannel collection techniques for medical debt involves aligning systems, workflows, and communication into a structured, coordinated approach. When done correctly, it enables agencies to scale outreach while improving recovery outcomes.

These are the key steps to implement an effective omnichannel strategy:
1. Assess Current Systems
Start by evaluating existing collections and communication systems. Identify gaps where channels are disconnected or workflows rely heavily on manual effort. This helps define what needs to be integrated or replaced to support a more coordinated approach.
2. Integrate Communication Channels
Bring SMS, email, voice, and IVR into a connected system. Ensure all channels work together instead of operating independently. This creates consistency in messaging and improves engagement across touchpoints.
3. Centralize Data
Create a single view of consumer interactions, balances, and payment history. This allows teams to deliver informed and relevant communication at every stage. It also reduces duplication and improves operational visibility.
4. Set Up Automated Workflows
Define triggers for outreach based on timelines, behavior, or account status. Automation ensures consistent follow-ups without increasing manual workload. This helps maintain momentum across the collection lifecycle.
5. Define Communication Sequences
Map out how and when each channel will be used across different stages. Ensure messaging is aligned and builds context over time. This creates a structured communication flow that guides users toward payment.
6. Embed Payment Options
Ensure every communication leads directly to a payment method. Integrate portals, payment links, and IVR to reduce friction. This shortens the gap between outreach and resolution.
7. Ensure Compliance Controls
Build regulatory safeguards into workflows and communication rules. This ensures outreach remains within legal boundaries across all channels. It also reduces risk while allowing teams to scale operations confidently.
8. Monitor and Optimize Performance
Track engagement, response rates, and payment conversions across channels. Use these insights to refine communication strategies and workflows. Continuous optimization ensures long-term effectiveness.
Implementation creates the framework, but performance depends on how consumers respond to communication. In the next section, we look at practical ways to improve response across multiple channels.
Suggested Read: Healthcare & Medical Debt Collection Software
Consumer response depends on how communication is delivered and experienced. Small changes in messaging, timing, and channel use can significantly impact engagement.
These are practical ways to improve engagement across channels:
Improving response rates requires more than better messaging alone. It depends on having the right systems to support coordination, automation, and visibility. In the next section, we look at how the right technology enables collection agencies to execute omnichannel collections effectively.
Tratta is a digital debt collection and payment orchestration platform designed for collection agencies, debt buyers, and law firms. It acts as an execution layer that connects communication, payments, and workflows while integrating with existing systems. This allows agencies with healthcare portfolios to manage collections in a structured, scalable, and compliant way.
The platform enables omnichannel collections for healthcare portfolios by combining coordinated communication, secure data handling, and patient-friendly experiences. It is HIPAA compliant, supports secure PII management, and delivers high account verification success rates through configurable verification methods.
It also provides a complete set of features that support end-to-end collection operations beyond healthcare-specific needs. The following features work together to automate workflows and improve payment outcomes across every stage of the collection process.
Core features include:
We support implementation with rapid onboarding, system integration, portal launch, and team training within 35 days. Our white glove service ensures ongoing support with responsiveness, attention to detail, and a commitment to long-term success.
Omnichannel debt collection for healthcare can fail when systems are disconnected, messaging is inconsistent, and patients are pushed through fragmented experiences. Instead of improving recovery, it creates confusion, reduces engagement, and increases compliance risk.
Tratta solves this by connecting communication, payments, and workflows into a structured, compliant system built for healthcare portfolios. It combines omnichannel outreach with transparent billing, flexible payment options, and secure data handling, helping agencies improve engagement and recovery without disrupting existing systems.
See how Tratta can optimize your healthcare collections and improve recovery outcomes. Book a demo today.
Healthcare collections involve complex billing, insurance adjustments, and patient confusion. Unlike other industries, balances may change over time, requiring clear communication, transparency, and flexible options to ensure accurate understanding and timely payments.
When patients clearly understand their bills, they are more likely to engage and pay. Transparent communication reduces disputes, builds trust, and shortens the time between outreach and payment completion.
Yes, consistent communication across channels reduces misunderstandings. When patients receive clear, aligned information and easy access to documents, disputes decrease, and resolution becomes faster and more efficient.
Accurate patient data ensures correct communication and successful outreach. Incomplete or incorrect data leads to failed contact attempts, delays, and lower recovery rates, making data quality critical for effective collections.
Automation and structured workflows help manage large volumes without increasing workload. By reducing manual tasks and standardizing processes, agencies can scale operations while maintaining consistent communication and recovery performance.